This is the 5th of a series of eight articles chronicling the development of Customized Ablation or Wavefront Directed Lasik. This column was written following the 2001 AAO meeting and was published in the
January 1, 2002 issue of Ocular Surgery News.
Customized Ablation: The Wave Moves Forward --- but a new LASEK procedure may prove to be the winner!
Technology UpdateIrving J. Arons
Spectrum Consulting
Over the past several years, beginning in June 1999, I have written extensively on the coming of customized ablations based on wavefront diagnoses. All of the laser companies have initiated international trials and several have now begun their U.S. clinicals, including Alcon, VISX, and Bausch & Lomb. LaserSight and Nidek plan to begin U.S. trials by year's end, while WaveLight and Asclepion-Meditec plan to begin U.S. trials early next spring. (Schwind Eye-Tech Solutions does not intend to enter the U.S. market.) That all begs the question -- is wavefront diagnostics necessary to get good results with today's laser systems? My eyes were opened to the great results being reported by several laser companies using standard or "classic" LASIK on the new upgraded laser platforms, especially with low to moderate myopes. With the vast improvement in eye trackers now used with today's improved laser systems, it is almost routine for most refractive surgeons to bring better than 90% of their low to moderate myopes to 20/20 UCVA, while having a large proportion obtaining even better uncorrected acuities of 20/16 or better. (See the early results obtained for two laser systems with improved eye trackers shown in Tables 1 and 2.) So, I ask again, is wavefront necessary? And the unequivocal answer is YES!
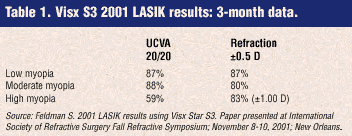

While not yet producing overall rates of 20/20 vision better than that is being obtained by "classic" LASIK yet, wavefront-guided ablations are being and will be used to correct irregular astigmatism and to correct past mistakes given either by decentered ablations, central islands, or other problems such as caused by scars or flaps. In addition, by correcting for spherical aberrations and some degree of higher order aberrations, the quality of vision can be improved, leading, for example, to improved mesopic or night vision. Then of course, there are those who desire "supervision", i.e., 20/16 or better UCVA. Those might include athletes, pilots and others for whom work-related super sharp vision is important. However, the vast majority of people will be satisfied with ridding themselves of eyeglasses or contact lenses for improved general distance vision. (Presbyopia is still mostly an unsolved problem, but as many as 85% of patients can do, and will do well with modified monovision -- with their dominant eye corrected for distance and the non-dominant eye for near.)
Wavefront diagnoses linked to laser ablation may not be the end all. Recent wavefront analyses of "top gun" pilots, whose vision was 20/12.5, was compared to other "top gun" pilots with normal 20/20 vision. It turned out that the wavefront analysis of the 20/12.5 pilots group showed significant amounts of higher order aberrations (primarily coma, a third order aberration) compared to the normal 20/20 group. If these supervision eyes had been corrected to rid them of the coma, it is likely they would have become 20/20 normal vision pilots! So, maybe some higher order aberrations are not necessary to correct. We still have a lot or work ahead of us to know what should and should not be corrected for.
In a debate held as part of the WaveLight meeting for their investigators, the question was asked, Wavefront or Not? And, although the ophthalmic audience in the end voted in favor of wavefront-guided ablation, this was probably because of the stature of the speaker (Prof. Theo Seilor), while the results obtained in the U.S. WaveLight clinical trials for the Allegretto laser without wavefront coupling (see Table 2, above), as presented by Guy Kezarian, were truly remarkable, and I would have been hard pressed to vote in favor of the need for wavefront diagnosis.
The Re-Emergence of LASEKThere has been quite a debate whether LASEK would result in a re-birth of PRK. Since I first wrote about this emerging technique a year ago, several refractive surgeons have turned to this procedure as their primary mode of surgery (Dan Durrie and Thomas Claringbold being among them). But, others have questioned the applicability of the procedure, especially with the epithelial cell death caused by the use of the alcohol solution to stiffen and loosen the epithelium from the underlying stromal bed. Well, I have good news.
My interest in writing about LASEK was piqued after hearing the results that Marguerite McDonald presented at the 2000 AAO meeting, where her Custom Cornea PRK patients had shown better results than those treated with LASIK following wavefront diagnosis. As she reported, her PRK patients eyes had much better UCVAs than did the eyes of her LASIK patients. This was probably due to the induced aberrations caused by creating the flap for LASIK. At the same meeting, actually at that year's ISRS Symposium, I first heard about Dr. Massimo Camellin's LASEK procedure, as reported by a couple of presenters. The combination of a better way of doing PRK, along with Dr. McDonald's better outcomes with customized PRK, led me to report on LASEK as a possible, even better way, of performing customized PRK.
Following the literature since my article, LASEK results in most other surgeons's hands have given mixed results. Then the wake up call came. In her Binkhorst award acceptance lecture at this year's AAO meeting, Dr. McDonald described a new LASEK approach and reported on the first results of patients she had treated with, as she described it, "gel-assisted LASEK". Instead of using alcohol to obtain epithelial peeling (with its accompanying death of many of the epithelial cells), she has found a better way to lift the epithelium. Using hydroxypropyl cellulose gel she can get both stiffening and separation of the epithelium, without causing cellular death. After using a specially designed spatula, and another specially designed tool for gel application, she is able to lift the epithelium and cut it into quadrants and move the quadrants out of the way for performing PRK onto the denuded stroma. Following the ablation, she is able to replace the epithelium (again with the use of the gel), and to protect the eye with a bandage contact lens during re-epithelization. Dr. McDonald reported that she had treated 40 eyes of 21 patients (two had only one eye operated on), with four eyes being treated for monovision, and not included in the UCVA study. With only 13 eyes available for two-week followup, she reported 85% were 20/20, and 100% were 20/25 or better. Now that's pretty good for a two-week followup for customized LASEK/PRK!
So, LASEK, that is gel-assisted LASEK, lives, and could be the answer to truly improved custom ablations!
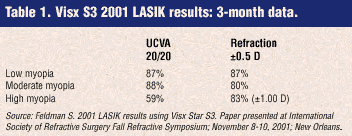



0 Comments:
Post a Comment
<< Home