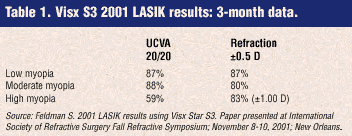This is the 6th of a series of eight articles chronicling the development of Customized Ablation or Wavefront Directed Lasik. This column was written following the pre-meetings before the 2001 AAO meeting and was published in the
January 15, 2002 issue of Ocular Surgery News.
Technology UpdateIrving J. Arons
Spectrum Consulting
AAO Refractive Pre-meetings Focus on LASIK, LASEK[LASIK results are improving with active eye trackers. LASEK may provide better results with wavefront-guided ablation. Other options seem far off in development.]
As I have done for several years, I attended the refractive pre-meetings held by the
International Society of Refractive Surgery (ISRS) and the
Refractive Surgery Interest Group (RSIG), prior to visiting the
AAO exhibit halls. This year, after looking at both programs, I decided to spend most of my time at the ISRS Fall Refractive Symposium. That two-day program was jam-packed with sessions of interest, and I had to pick and choose carefully in order to get a good sampling of what is new in refractive surgery.
First Day of ISRSJust to give you an idea of what I mean, the opening morning alone at the ISRS meeting had three sessions I wanted to attend -- Thermokeratoplasty & Non-excimer Lasers (covering laser thermokeratoplasty using both the
Sunrise [holmium] and
Rodenstock [diode] lasers, the
IntraLase femtosecond laser, and conductive keratoplasty using the
Refractec Viewpoint CK system); Laser Delivery and Profile Debate (covering eyetrackers, treatment zones sizes, and results obtained with several of the laser systems using the new eyetrackers; and the latest version of
Catch the Wave -- with presentations by most of the refractive laser companies describing the latest versions of their lasers and diagnostics. (The early morning presenters were
Alcon and
Nidek.) And that was just the early morning sessions.
The late morning sessions covered the use of LASIK for correcting hyperopia with and without astigmatism (which also snuck in the latest
Leeming Survey of Trends in Refractive Surgery in the United States: The 2001 ISRS Survey -- more on this later), and a session on microkeratomes, with nine speakers discussing their favorite keratome. The Catch the Wave presenters during this session were
VISX and
LaserSight.
The early afternoon session had a discussion on refractive IOLs, with several speakers debating the merits of use of phakic IOLs, and including a session on a new laser adjustable IOL; a session on Worst Case/Best Save Video Groundrounds, which included several presentations on LASEK; while Catch the Wave continued with three of the small spot scanning laser presentations (by
Asclepion-Meditec,
WaveLight, and
Bausch & Lomb).
The late afternoon included a discussion of LASIK Complications and a session titled Diagnostic Wavefront/Optical Aberrations, which included a face-off between the various measurement systems -- Hartmann-Shack aberrometry (
Alcon,
Asclepion-Meditec,
Bausch & Lomb, and
VISX), ray tracing (
Tracey), scanning slit refractometer (
Nidek), and Tscherning (
WaveLight and
Schwind); versus corneal mapping using AstraMax (
LaserSight), Orbscan (
Bausch & Lomb), and other topographers. The real question asked -- is wavefront measurement necessary, or is topographical measurement enough?
And that was just the first day of the meeting.
Second Day of ISRSOn the second day, the early morning sessions included meetings on Wavefront Technology and Custom Ablation -- a face-off of the various laser systems and their approaches to wavefront-guided custom ablations; and another section on topography versus wavefront. The competing early morning session was on refractive implantable devices, including talks on Intacs, intracorneal implants for hyperopia (the PermaVision lens from
Anamed), the Ferrara intracorneal rings, and talks on implantable IOLs for hyperopia.
The late morning sessions included Presbyopia Correction, with discussions of scleral bands (
Presby Corp.), laser ablation (
SurgiLight), anterior sclerotomy, myopic LASIK with monovision, LTK for monovision, and talks on two of the accommodating IOLs (the AT-45 from
C&C Vision and the 1CU from
Human Eyes); along with a second session on LASIK Complications.
The afternoon sessions included one on management issues, Re-inventing Yourself as a Refractive Surgeon: What it Takes in 2001; and a session on LASIK Enhancement and Lamellar Surgery.
In looking over the RSIG meeting program, a number of the same topics were covered, including LASIK techniques and complications; PRK and Intracorneal Implants; Presbyopia; Surgical Correction of Hyperopia; IOLs in Refractive Surgery; and Refractive Lasers and Aberrometers.
OverviewIn order to cover as many bases as possible, I have organized this article to include the latest information by type of correction, i.e., what is happening in the correction of myopia, hyperopia, and presbyopia. The report mainly covers laser approaches, but includes, where appropriate, non-laser techniques under development to replace/displace the laser approaches, such as inlays (Permavision from Anamed) and heated tips (ViewPoint CK from Refractec) for hyperopia, and accommodating IOLs and surgical techniques (Presby Corp.) for presbyopia. Included in the laser discussions are excimer-based procedures, as well as those being done with holmium (Sunrise's LTK), erbium (SurgiLight's presbyopia reversal), and femtosecond devices (IntraLase's microkeratome replacement today, and possible refractive application in the future).
Current Correction of MyopiaAccording to the latest survey data from
Market Scope, close to 94% of ophthalmologists are using standard or "classic" LASIK for correcting low myopia (up to 3 diopters); almost 99% use LASIK for moderate myopia (up to 5 diopters); while 91% use it for high myopia (over 7 diopters) -- the rest using phakic IOLs (5%) or some other technique. The percentages are just as high for correcting myopia with astigmatism. Thus, the question to be answered at this year's meetings was, is there anything coming along that might replace "classic" LASIK?
And there were some answers. The use of eyetrackers are leading to some spectacular results with LASIK. The newer laser systems with improved eyetrackers seem to be obtaining excellent results. As shown in my accompanying Customized Ablation article (#5 in this series), the reported results for just two of the newer laser systems, the VISX Star S3 with Active Trak, and the Wavelight Allegretto, also with an active infrared tracker, compare very well with the data obtained with the initial results obtained in the wavefront customized ablation trials reported to date. The use of eyetrackers leads to better centration (with no decentration) and the ability to place blend zones where they add to better quality vision (reduction of glare and halos in night vision).
Future Correction of MyopiaThe next question is how much better will the results be with either wavefront or corneal topographers added to the systems. That answer was not as clear. Two of the companies have topography systems combined with their wavefront devices -- Bausch & Lomb's Zyoptix Zywave wavefront along with its Orbscan IIZ topographer and Nidek's NAVEX OPD-Scan, which combines topography with retinoscopy to provide total eye aberrations. In addition, LaserSight has developed its AstraMax stereotopography system which is linked to their new CIPTA software to provide oblate corneal ablations. (Only Alcon and VISX do not have a built-in topographer.) I was not able to obtain clinical data on these systems, but scuttlebutt in the halls of the meeting suggested that all were providing improved results when compared to "classic" LASIK.
All of the laser manufacturers now have some sort of active eye trackers, and all but LaserSight have working wavefront devices. So far, only the Asclepion, Schwind, WaveLight and Alcon systems are directly linked to their lasers. But all companies have plans to do that and, with the systems in use today, it is a simple task to perform the wavefront analysis, copy it to a disc, and place the disc into the laser to perform the ablation. Also noted in the table is the status of U.S. clinical trials for custom ablations. Alcon and B&L (with their international data) appear to be in the lead, with VISX about six to eight months behind. All of the other companies are still in their planning stages.
So, the real question is -- if "classic" LASIK with the improved laser systems is working so well, do we need wavefront? And, as I've said, that answer is not clear. Wavefront-guided ablations will be used to correct previous problems, including decentered ablation, uncleared central islands, and irregular astigmatism. It is expected to improve the quality of vision, especially for those people suffering from poor night vision, and to minimize induced aberrations, as well as correcting higher order aberrations such as third-order aberrations coma and trefoil. But, there is the problem of how much higher order aberrations should be corrected? As related in Customized Ablation article, in a study of Navy Top Gun pilots, a comparison of higher order aberrations showed that those pilots with 20/12.5 acuity had some degree of coma, while those with normal 20/20 acuities, had less. Would we turn 20/12.5 pilots into 20/20 pilots if we corrected their higher order aberrations?
The first answers are ambiguous. As reported by Coleman Kraff, MD, some surgeons are getting excellent results, but others haven't yet hit their mark. (See the Postop Wavefront Outcomes table in the Customized Ablation article.)
In order for wavefront-guided ablations to provide for minimized individual aberrations, there is the need to accurately register the eye between the capture of the diagnosis and the treatment, and preferably this should be done in three axes. There appears to be a lot of work ahead before wavefront-guided ablations become the norm.
One last point. LASIK, even with wavefront, gives more aberrations rather than fewer. PRK, as shown in Marguerite McDonald's study of wavefront-guided PRK vs. LASIK studies last year showed that her PRK patients routinely had better acuities than did her LASIK patients. Thus the impetus for LASEK. But, the results reported to date for LASEK have been a mixed bag, some doctors reporting excellent results, while others have reported problems due to the alcohol solution used to lift the epithelium causing cell deaths, haze, and regression.
Now, as reported in the Customized Ablation article, Dr. McDonald has done it again. In her Binkhorst Lecture acceptance speech, she described what she calls "gel-assisted LASEK". Using hydroxypropylcellulose gel, she found that she could "stiffen" the epithelium and lift it from its stromal bed, and then cut it into quadrants that can be lifted outward away from the ablation zone, allowing PRK to be performed on the stroma. Again using the gel, she was able to push the epithelium quadrants back onto the cornea, and using a bandage contact lens, get re-epithelization without cellular loss. She believes that flap-free LASEK is a safer alternative to LASIK.
LASIK/LASEK Refractive AlternativesTo quickly answer the question, what lays beyond the answers shown above? Not much. Intralase with its femtosecond laser to perform intrastromal ablation -- the removal of tissue within the stroma by making two passes at different levels -- is still quite a ways off. Previous attempts to do this by both
Intelligent Surgical Laser (picosecond laser) and
Phoenix Laser Systems (with a Q-switched YAG) in the late 1980s were unsuccessful. As far as I can tell, only early experiments have been performed, and it will probably be some time before human trials are conducted. The company strategy is first to establish a beachhead as a microkeratome, then seek approval to treat presbyopia, and finally to go after myopia approval.
I do not see clear lens extraction, especially for low to moderate myopes as an alternative to refractive surgery.
As for the solid-state laser from
Q-Vis, after speaking to company representatives at the meeting, it appears that this company is a long way from establishing a beachhead in the U.S. The company is just starting Phase III clinical trials, so is at least 12-18 months away from filing their PMA. There is also the question of carcinogenesis caused by the 213 nm wavelength. As I recall from my early days in excimer refractive surgery, that question had been raised when JT Lin first proposed a solid-state quintupled YAG operating at 213 nm. I'm not sure it was ever fully resolved.
There is however, a fly in the ointment.
Ciba Vision has recently had a new extended wear contact lens approved, and
Bausch & Lomb has followed suit, with a second approved lens. These could prove to be viable alternatives to surgery. Back in the mid-seventies, when the first extended wear lenses became available, they took the public by storm -- some of you may recall the
CooperVision TV ad that proclaimed -- "I can see beyond my bedcovers!" However, corneal ulcers and other problems soon stopped that generation of lenses in their tracks. But, these new lenses are truly oxygen permeable and have probably overcome all of the earlier problems. So, I advise you to carefully watch how well they are accepted.
Current Correction of HyperopiaAgain, according to the Market Scope Survey of Refractive Surgeons, almost every surgeon chooses LASIK for the correction of low or moderate hyperopia, with or without astigmatism -- in the high 80%s. Only about 8% of surgeons use Sunrises' LTK system, about 1% still use PRK, with 4% (for low hyperopia) and 16% (for moderate hyperopia) choose some other means (undefined). Only for high hyperopia correction, do 20% of surgeons turn to phakic IOLs, while 21% still use LASIK, and 63% choose some other means.
The ISRS Survey showed similar results. For +1 hyperopes, 70% of survey respondents chose LASIK, 17% said they would use either LTK or CK; for +3 hyperopes, 84% chose LASIK and only 2% said they would use LTK or CLE (clear lens extraction); for +5 hyperopes, 29% chose LASIK, 39% said their choice was CLE, while 30% said they would wait for something else.
Based on what I picked up at the sessions, the two laser systems approved for hyperopia (LadarVision and Star S3), with their working eyetracker systems, are achieving very good results for hyperopia and hyperopia with astigmatism. The feeling was that these newer systems were giving 3 to 4 times improvement over those systems without the eyetracker. For that reason, few ophthalmologists appear to be interested in trying the Sunrise LTK system, which has apparently fallen out of favor. There was however, much interest in the Refractec ViewPoint CK system, especially at its very low price point of $45,000 for the unit and approximately $100-$150 for the disposable tips, one used for each eye.
Future Correction of HyperopiaOn the horizon, the only other new means for correcting hyperopia is the Anamed PermaVision Lens. This unique 78% hydrogel lenticle, with the same refractive index as the cornea, and which is only 30-60 microns thick, appears to provide adequate fluid and nutrient flow to keep the cornea healthy. It is used for correcting from +1 to +6 diopter of hyperopia, by opening a flap in the cornea, inserting the lens, and closing the flap. In the international clinical study, in sixty patients, the average starting spherical manifest spherical equivalent was +3.52 diopters. Of 14 patients examined after six months, the SME was down to +0.58 diopters. Immediately postop, the patients were about -0.5 myopic, and they drifted to plano over two to three weeks.
An inversion problem with insertion of the lens has apparently been overcome with the use of a new applicator delivery system. The company has received CE approval for marketing in Europe. U.S. clinical trials are expected to begin by the end of this year.
I did not sit in on any of the sessions covering the phakic IOL lenses, and therefore, will not comment on them in this report.
Current Correction of PresbyopiaAs listed by John Hunkeler, there are a bevy of options for the correction of presbyopia: these include monovision, pseudo accommodation, and multifocal vision. Among the surgical options are monovision LASIK, multifocal corneal ablation, monovision with LTK or CK, scleral relaxing incisions, scleral expansion bands, laser scleral ablation, and lens exchange using the Array multifocal IOL, and accommodating IOLs. Of course, he left out no-line eyeglasses and multifocal contact lenses.
Of all the options, other than LASIK monovision, probably the insertion of the Array multifocal IOL has had the best results to date. While the jury is still out on the accommodating IOLs from at least three manufacturers -- the AT-45 CrystaLens from C&C Vision, the Human Optics 1CU, and an unnamed lens under development by Quest Vision.
Future Correction of PresbyopiaOf the non-monovision surgical options, ancillary scleral relaxation incisions don't work. Just cutting the sclera, in an RK-like fashion, quickly regresses and leaves the patient with no change in near vision. Scleral expansion bands do seem to provide some near vision ability for about 70% of the patients tried to date. While laser scleral ablation, which appears barbaric when witnessed, has had good results in some doctors hands, others have not fared as well. More trials are needed with both of these latter techniques to see if they will really work in the non-specialist's hands.